Millions of people in the United States suffer from dry eye disease every year. This can be a frustratingly tough disorder to manage as it has many potential causes. It is important that you address dry eye before it becomes too severe and causes long-lasting damage to your eyes. How do you know if you actually have dry eye disease, though?
At-home evaluation
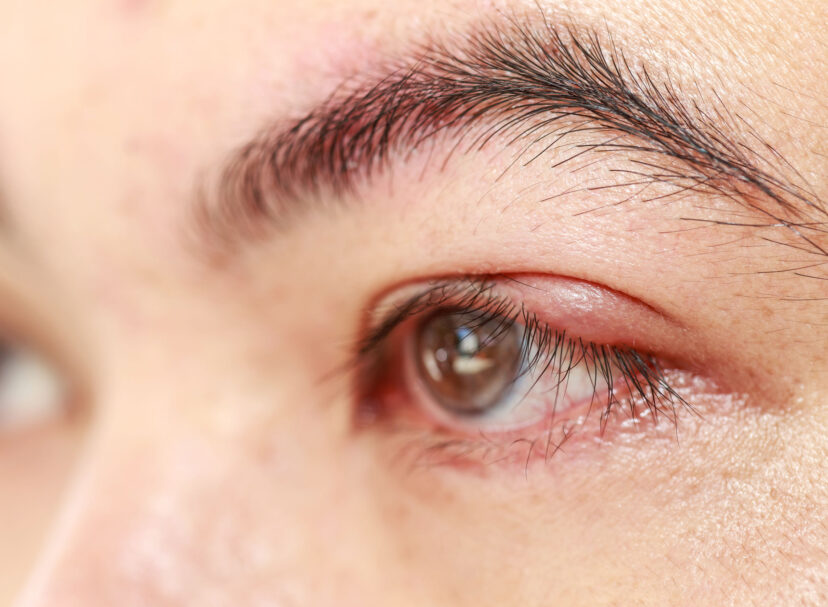
You likely have already experienced some of the tell-tale symptoms of dry eye diseases. Signs that you may be suffering from dry eye disease include most of the usual eye irritations: dryness, redness, watering, tiredness, itching, soreness, stinging, or burning, as well as blurred vision or difficulty focusing. You may also be extra sensitive to light or feel as though something is stuck in your eye. If you are experiencing some or all of these symptoms, dry eye is likely.
Although not an accurate diagnosis, a self-evaluation can point you toward some helpful over-the-counter remedies. However, not everyone with dry eye experiences all of these symptoms, and nobody feels them in the exact same way. If you suspect you have dry eye disease, the best course of action would be to visit your eye doctor. They can make an accurate diagnosis and provide you with the best treatment recommendations.
Clinical diagnosis of dry eye
Eye doctors have a variety of diagnostic tools to help identify dry eye disease in patients. They will start by examining your eyes visually, checking how frequently you blink and looking for any inflammation. A “slit lamp” is used for these exams; you may already be familiar with these small, high-intensity lights that are used routinely during optician visits. In severe cases of dry eye, your doctor may find damage on your cornea.1
Another commonly-used assessment is the “Schirmer test,” in which the water content of your eyes is measured. During this test, the ophthalmologist will touch a piece of filter paper to your lower eye and measure how far the water is absorbed into the paper. Fluid absorption below a certain threshold indicates you don’t have sufficient liquid on the surface of your eyes.2
Your eye doctor might also perform a test to evaluate the quality of your tear film. Your tears are normally protected from evaporation or spilling over by a layer of lipids and proteins. A common test for this is “tear film breakup time” or TFBUT. For this test, the doctor will put a special dye called fluorescein in your eye, then have you hold your eye open without blinking for around 30 seconds. If they see your tear film dissipate too quickly, a dysfunction of your meibomian glands may be the source of your dry eye.3
Next steps
Your doctor will recommend specific treatments for dry eye depending on your particular case. In the meantime, you may find temporary relief from symptoms of dryness by using lubricating eye drops. And of course, as with any eye disorder, maintaining proper ocular hygiene is key. It can help in reducing inflammation, removing underlying infections, and keeping dry eye from recurring. Check out Cliradex wipes and foaming cleansers for safe, natural products that target a broad range of dry eye-causing problems.
Resources:
- Kanellopoulos AJ, Asimellis G. In pursuit of objective dry eye screening clinical techniques. Eye and vision (London, England). 2016;3:1.
- Zeev MS, Miller DD, Latkany R. Diagnosis of dry eye disease and emerging technologies. Clinical ophthalmology (Auckland, NZ). 2014;8:581-590.
- Messmer EM. The pathophysiology, diagnosis, and treatment of dry eye disease. Deutsches Arzteblatt international. 2015;112(5):71-81; quiz 82.